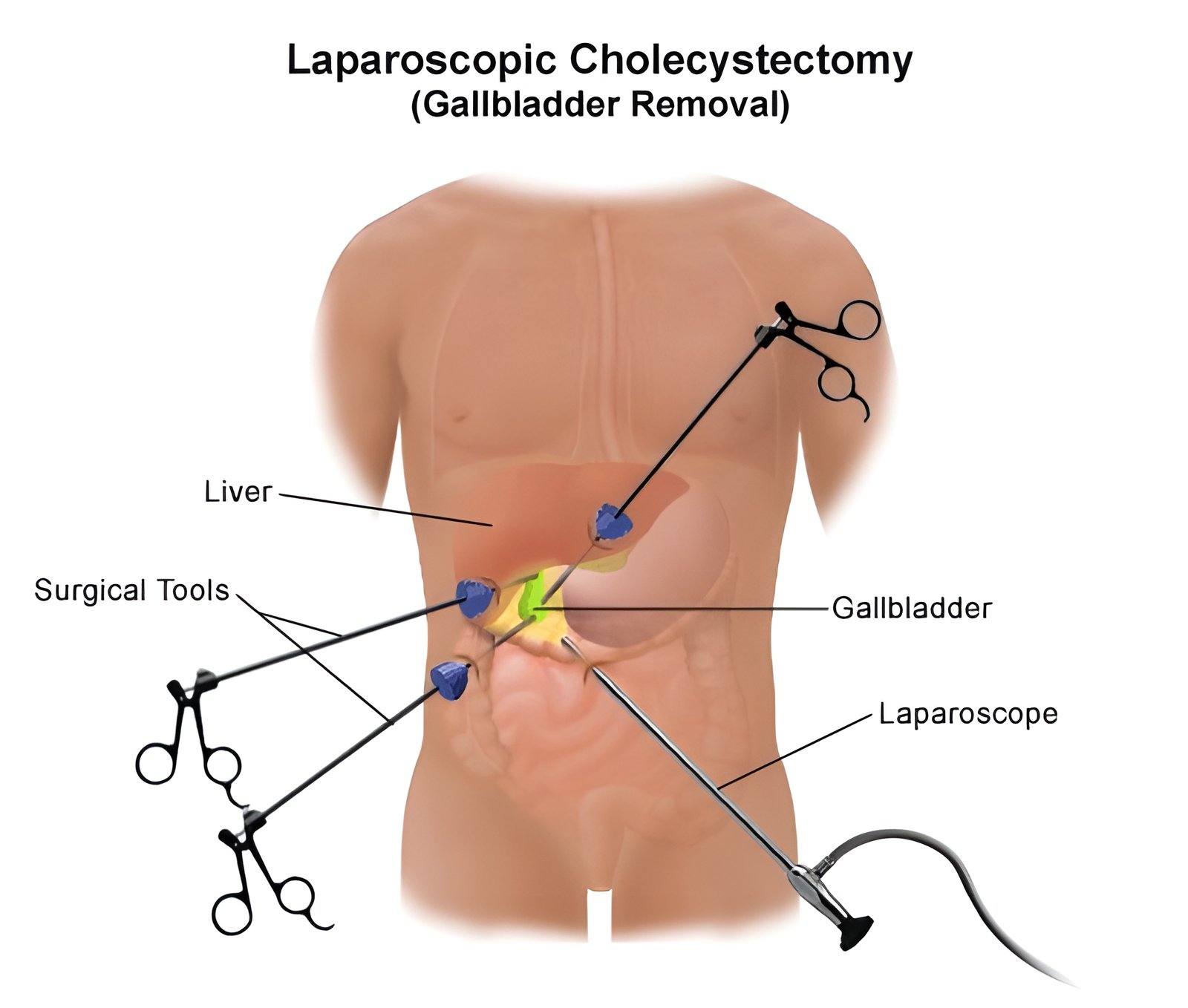
Laparoscopic Gallbladder Removal
Understanding the Gallbladder and Its Function
The gallbladder is a small, pear-shaped organ located beneath the liver, playing a crucial role in the digestive system. Its primary function is to store bile, a digestive fluid produced by the liver. Bile aids in the digestion and absorption of fats in the small intestine, emulsifying dietary fat to facilitate its breakdown. When food enters the duodenum, the first part of the small intestine, the gallbladder contracts and releases bile through the bile ducts into the digestive tract, ensuring an efficient digestive process.
Despite its important role, the gallbladder is susceptible to various disorders that can disrupt its function. One of the most common conditions is the formation of gallstones, which are solid particles that develop from bile components, primarily cholesterol and bilirubin. These stones can vary in size and may cause significant pain or complications if they obstruct the bile ducts. Another prevalent disorder is cholecystitis, an inflammation of the gallbladder often resulting from gallstones blocking the cystic duct. Symptoms of gallbladder disorders typically include abdominal pain, nausea, and jaundice. When these conditions arise, they can lead to further complications and often necessitate surgical intervention.
Gallbladder removal, or cholecystectomy, may be required when conservative treatments fail or when symptoms significantly impair a patient’s quality of life. Understanding the role of the gallbladder and the various conditions that can affect it is essential for recognizing the importance of surgical procedures to address gallbladder dysfunction. By familiarizing oneself with the anatomy and function of the gallbladder, individuals can better appreciate the reasons for surgical removal in cases where the gallbladder fails to perform its vital digestive roles efficiently.
The Laparoscopic Gallbladder Removal Procedure
The laparoscopic gallbladder removal procedure, also known as laparoscopic cholecystectomy, begins with a thorough preoperative assessment. This assessment generally includes blood tests, imaging studies such as an ultrasound, and discussions regarding the patient’s medical history. Ensuring the patient understands the procedure and consents to the surgery is essential. Preoperative instructions typically involve fasting and possibly adjusting medications to minimize risks during and after the operation.
On the day of the surgery, the patient is positioned on the operating table and administered anesthesia. Once the patient is sedated, the surgeon initiates the procedure by making four small incisions in the abdomen. These incisions allow access for the laparoscope, a thin tube equipped with a camera, as well as other surgical instruments. The laparoscope transmits images to a monitor, providing the surgeon with a clear view of the gallbladder and surrounding organs.
The surgeon carefully dissects the gallbladder from its attachments using specialized laparoscopic tools. This phase requires precision to avoid injuring nearby structures, including the bile ducts and blood vessels. Once dissected, the gallbladder is removed from the body through one of the incisions, often using a technique called retrieval bagging, which minimizes spillage of bile or stones. Dr. Imran Hussain Andrabi places emphasis on meticulous technique during this phase, ensuring patient safety and optimal outcomes.
After the gallbladder is removed, the surgeon thoroughly inspects the surgical site for any residual stones or complications. The incisions are closed with sutures or surgical adhesive. One notable advantage of laparoscopic techniques, as practiced by Dr. Andrabi, is the significantly reduced recovery time compared to traditional open surgery. Patients often experience less pain, smaller scars, and a quicker return to normal activities, making laparoscopic cholecystectomy a preferred choice for gallbladder removal.
Postoperative Care and Recovery
After laparoscopic gallbladder removal, also known as cholecystectomy, patients can generally expect a few days of recovery before resuming normal activities. Typically, the initial phase of recovery lasts about one to two weeks. However, complete healing can take up to six weeks depending on individual health and adherence to postoperative care guidelines. Understanding the typical recovery timeline is essential for managing expectations and ensuring a smooth transition back to daily life.
In the days immediately following the surgery, patients may experience some discomfort, including bloating, shoulder pain, and fatigue. These symptoms, while common, should gradually improve. It is crucial to monitor the surgical site for any signs of infection, such as increased redness or discharge, and to report any unusual pain or persistent symptoms to the healthcare provider. Adequate hydration and rest are also crucial during this phase.
Dietary modifications play a significant role in recovery post-cholecystectomy. It is advisable to introduce a low-fat diet gradually, as high-fat meals can lead to digestive discomfort. Many patients find it beneficial to consume smaller, more frequent meals instead of large dishes, allowing the digestive system to adjust without overwhelming it. Incorporating plenty of fruits, vegetables, and whole grains can also promote recovery. Patients should remain attentive to their body’s responses and adjust their diets accordingly.
Follow-up care with the healthcare provider is vital to ensure proper healing and address any concerns that may arise. Regular check-ups can help monitor healing progress and manage any potential side effects effectively. In addition, lifestyle changes, such as engaging in light physical activity to encourage circulation and compliance with dietary recommendations, will support overall recovery.
In conclusion, following laparoscopic gallbladder removal, patients must prioritize adequate care, embrace dietary changes, and remain vigilant about follow-up appointments, all of which foster a successful recovery journey.
Expert Insights from Dr. Imran Hussain Andrabi
As a seasoned surgeon specialized in laparoscopic procedures, I have seen a significant evolution in the techniques and technology associated with laparoscopic gallbladder removal, also known as laparoscopic cholecystectomy. My experience in this field has led me to recognize the critical importance of patient selection, which must be tailored to each individual’s condition and needs. Not every candidate is ideal for laparoscopic surgery; factors such as anatomy, coexisting health issues, and the presence of complications like severe inflammation or infection play a vital role in determining the appropriateness of this minimally invasive approach.
The advancement of laparoscopic techniques has revolutionized how we perform gallbladder removals. The adoption of high-definition imaging and enhanced instrumentation has greatly improved both the safety and efficacy of the procedure. These innovations not only allow for a clearer view of the surgical area but also enable more precise manipulations, reducing the risks associated with surgery. This has led to shorter recovery times, reduced postoperative pain, and fewer complications, benefiting the patient significantly.
Another critical aspect of my practice is personalized care. Each patient presents a unique clinical picture that requires a tailored approach. I firmly believe in the importance of discussing all available options with my patients, ensuring they understand the benefits and risks associated with laparoscopic gallbladder removal versus traditional methods. By fostering open communication and establishing an individualized treatment plan, we can achieve the best possible outcomes for our patients. It is this holistic approach combined with the advancements in laparoscopic techniques that have defined my practice and contributed to my commitment to providing high-quality surgical care.